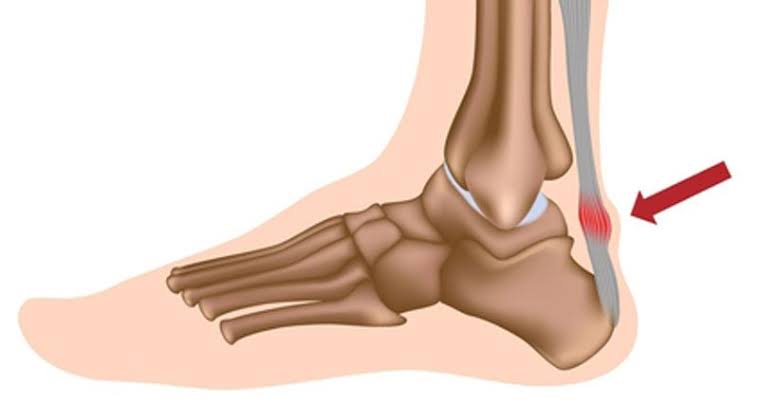
The Achilles tendon joins the muscles of the calf to the bone of the heel and runs down the lower leg. This tendon can become inflamed when put under excess pressure. This is tendinitis in Achilles.
Achilles tendon is the body ‘s strongest tendon. It can withstand great strength but it is still vulnerable to injury.
Achilles tendinitis, or tendonitis, is typically the result of microtears that occur in the tendon during strenuous, high-impact exercise like running.
The tendon can get ruptured or torn untreated. Treatment may include resting or modifying an exercise regimen in mild cases but more serious cases may require surgery.
Treatment

The therapy aims at alleviating discomfort and reducing swelling. Treatment option would depend on the severity of the condition, and whether or not the individual is a professional athlete.
A combination of strategies will likely be suggested by your doctor.
Treatment strategies for Achille tendinitis include:
- Ice packs: Applying these to the tendon, when in pain or after exercising, can alleviate pain and inflammation.
- Rest: This gives the tissue time to heal. The type of rest needed depends on the severity of the symptoms. In mild cases, it may mean reducing the intensity of a workout, but severe cases might require complete rest for days or weeks.
- Elevating the foot: Keeping the foot raised above the level of the heart can reduce swelling.
- Pain relief: Nonsteroidal anti-inflammatory drugs (NSAIDS), such as ibuprofen, can reduce pain and swelling. People with asthma, kidney disease, or liver disease should first check with a doctor.
- Steroid injections: Cortisone, for example, can reduce tendon swelling, but it has also been associated with a greater risk of tendon rupture. Giving the injection while scanning the area with ultrasound can reduce this risk.
- Compression bandages and orthotic devices: Ankle supports and shoe inserts can aid recovery as they take the stress off the tendon. Heel lifts, which move the foot away from the back of the shoe, may help patients with insertional Achilles tendinitis.
- Extracorporeal shockwave therapy (ESWT): High-energy shockwaves are used to stimulate the healing process. Results have not been consistent, but if other measures do not work, it might be worth trying before opting for surgery.
It usually takes between a few days and 6 weeks for tendinitis to heal.
Surgery
Surgery can remedy the tendon damage caused by Achilles tendinitis. The American Academy of Orthopedic Surgeons (AAOS) suggests surgery only if the pain lasts for six months or longer.
The most common treatment is the regression of gastrocnemias. That involves lengthening one of the two muscles that make up the calf to allow a broader range of motion to the ankle.
Stretches and exercises
A physiotherapist may teach stretching exercises to improve flexibility and increase the strength of the calf.
Here are two exercises, suggested by the AAOS.
Calf stretch
- Lean forward with your hands against a wall.
- Have one foot on the ground, with the leg straight, and one foot in front of it, with the knee bent.
- Push your hips toward the wall and hold for 10 seconds.
- Relax and repeat 20 times for each foot.
Bilateral heel drop
- Stand with the front half of your foot on the stair and the heel off, holding a rail to make sure you are balanced and will not fall.
- Slowly lift your heels and lower them as far as you can.
- Repeat 20 times.
Both exercises have to be carried out slowly and in a controlled way. Having them done quickly can increase the damage.
This can help heal the Achilles tendon and prevent future injury. Physical therapy for non-insertional Achilles tendinitis is normally more effective.
Symptoms
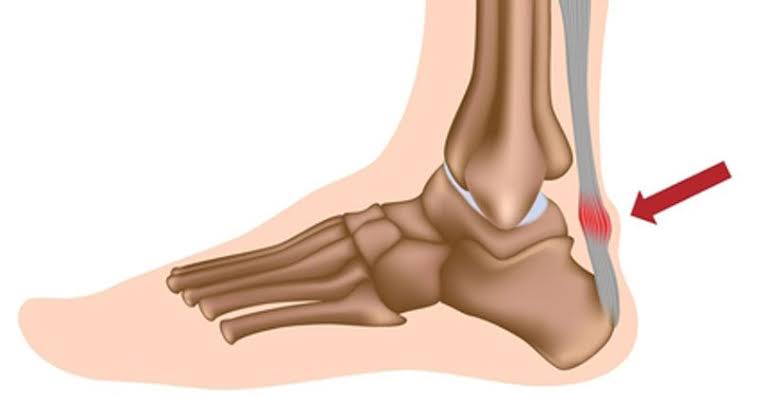
Achilles tendinitis’ key symptom is a gradual accumulation of pain that worsens over time.
In addition, the person may notice the following:
- The Achilles tendon feels sore a few centimeters above where it meets the heel bone.
- The lower leg feels stiff, slow, or weak.
- A slight pain appears in the back of the leg after running or exercising and becomes more severe.
- Pain in the Achilles tendon occurs while running or a couple of hours after.
- Pain is greater when running fast, for a long time, or when climbing stairs.
- The Achilles tendon swells or forms a bump.
- The Achilles tendon creaks when touched or moved
Diagnosis
These and other similar symptoms feature in a number of conditions, so precise diagnosis requires medical advice.
A specialist should inquire about the signs and do a physical exam. They will touch the back of the ankle and tendon gently to find the pain or inflammation source.
The doctor will also check the foot and ankle to see whether it impairs the range of motion and endurance.
For example, an imaging examination, an x-ray, MRI, or ultrasound scan, can help remove other potential causes of pain and swelling and assess any damage to the tendon.
Possible complications
Achilles tendinitis may cause tendinosis of Achilles, a degenerative condition in which the tendon structure changes and becomes susceptible to serious damage. The tendon can tear, causing great pain.
Tendinitis and tendinosis are conditions which differ. Tendinitis involves inflammation, while tendinosis is a cellular-level degenerative process, and inflammation is not present. Sometimes the tendinosis is misdiagnosed as tendinitis. Having the correct diagnosis leads to better treatment.
Causes
Achilles tendinitis can grow in different ways. Others can be prevented more quickly than others, but being conscious of them can help with early diagnosis and help prevent serious injury.
Achilles tendinitis Non-insertional is more common in younger, more active individuals. The fibers in the center of the tendon begin to break down, thicken and swell.
Achilles tendinitis insertional is not necessarily activity related. As it inserts into the heel bone it affects the lower portion of the tendon.
Causes of Achilles tendinitis include:
- Using incorrect or worn out shoes when running or exercising
- Not warming up properly before exercise
- Increasing intensity of exercise too quickly, for example, running speed or distance covered
- Prematurely introducing hill running or stair climbing to an exercise routine
- Running on hard or uneven surfaces
- The calf muscle is injured or has little flexibility, putting more strain on the Achilles tendon
- Sudden intense physical activity such as sprinting for the finish line
Differences in anatomy of the foot, leg, or ankle can also cause tendinitis of Achilles. Flat feet or fallen arches may put the tendon under pressure.
Bone spurs are extra growths in bones where the tendon joins the bone. These are able to rub against the tendon of Achilles, causing damage and discomfort.
Patients taking antibiotics with fluoroquinolone may have a higher risk for tendinitis and tendon rupture. In 2008, the FDA requested that the prescribing information for Cipro, or ciprofloxacin, Factive, or gemifloxacin and others be added to a boxed warning.
The risk of injury does not disappear when the dosage stops. People reported having tendon problems several months after starting using the medication.
Outlook
Recovery depends on the severity of a tendinitis.
The AAOS says that even with early treatment, it can take several months for the pain to go away.
If the pain does not resolve within 6 months, this may require surgery. Many who undergo surgery will not be able to return to competitive sports or run for a minimum of 12 months. Some aren’t going back to their sport.
The best way to avoid long-term complications is through prevention and early diagnosis.
Prevention

Achilles tendinitis can not be completely prevented, but by being aware of the possible causes and taking precautions can reduce the risk of it developing.
These include:
- Varying exercise: Alternating between high-impact exercises, such as running, and low-impact exercise, for example, swimming, can reduce stress on the Achilles tendon on some days.
- Limiting certain exercises: Too much hill running, for example, can put excessive strain on the Achilles tendon.
- Wearing the correct shoes and replacing them when worn: Shoes that support the arch and protect the heel create less tension in the tendon.
- Using arch supports inside the shoe: This can help if the shoe is in good condition but does not provide the required arch support.
- Gradually increasing the intensity of a workout: Achilles tendinitis can occur when the tendon is suddenly put under too much strain, so warming up and increasing the level of activity gradually gives the muscles time to loosen up, and this puts less pressure on the tendon.
It is important to stretch and warm up before and after exercising. Stretching helps maintain flexibility in the Achilles tendon, so there is less chance of developing tendinitis. Everyday stretching, including days of rest, will further enhance flexibility.