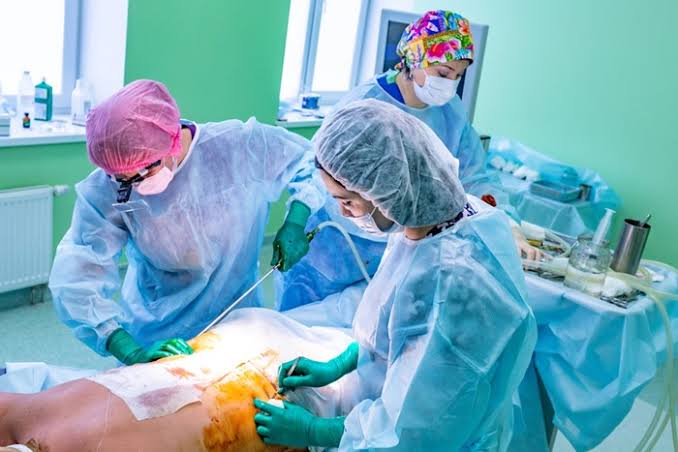
A biopsy is a method of diagnosing illnesses. A doctor extracts a sample of tissue or cells, typically under a microscope, to be examined by a pathologist.
A pathologist is a specialist qualified to examine a tissue sample under a microscope for signs and extent of illness.
Tissue is usually taken from a living subject for a biopsy.
The word biopsy comes from the Greek words “bios,” meaning “life,” and “opsis,” meaning “a view.” They mean “to view life” together.
Meaning

A biopsy can be excisional or incisional, depending on the goal:
- An excisional biopsy is the surgical removal of a whole lump or targeted region
- An incisional biopsy, or core biopsy, requires taking a tissue sample
There are different types of biopsy.
Scrape: The cells are separated from the surface of the tissue, such as the inside of the womb or the neck of the mouth or the cervix, for example. It is also used, widely known as pap smears, in cervical cancer screening. It can be used to confirm the existence of fungal skin infections.
A punch biopsy: A punch is a round-shaped knife which is used to cut and extract a tissue disk. This is used to collect a sample of skin tissue and can also be used to check for inflammation in order to check for malignancy or cancer.
A needle biopsy: A needle, typically made of liquid, is used to extract a sample. For a core biopsy, a large needle is used, while a thin one is used for a fine-needle aspiration biopsy (FNAB). It is also used for sampling breasts and thyroids.
A capsule biopsy: This is used to take a sample from the intestine.
Stereotactic biopsy: Samples are taken from the brain to find the biopsy site using stereotactic surgery. In order to locate small targets within the body, a stereotactic system uses three-dimensional coordinates.
Colposcopic biopsy: This is used to test a patient who has had a pap, or cervical, abnormal smear. The colposcope is a close-focus telescope that helps the physician to see in detail the areas of the cervix.
Endoscopic biopsy: In order to collect a sample, an endoscope is used. An endoscope is a long, thin, lighted optical instrument used to get deep inside the body and analyse or operate on organs.
Specially adapted endoscopes include a bladder cystoscope, a kidney nephroscope, a bronchial or lung bronchoscope, a speech box or larynx laryngoscope, and an ear otoscope.
Almost any organ can be biopsied.
Uses
We may not visualize the organs or tissues within our body, but by presenting a piece of tissue for analysis, a biopsy helps to make a diagnosis. Cancer is mostly associated with biopsies, but they may be used to identify various diseases and to see how far a disease has advanced. Sometimes, they help rule out cancer.
Conditions where there may be a role for a biopsy include:
- Cancer: If the patient has a lump or swelling of no clear cause anywhere in the body, the only way to ascertain whether or not it is cancerous is through a biopsy.
- Peptic ulcer: A biopsy will help a doctor decide if a non-steroidal anti-inflammatory drug (NSAIDs) is causing ulceration . To test patients with malabsorption, anemia, or celiac disease, a small bowel biopsy can be used.
- Diagnosis of liver disease This may help the health care provider detect liver tumors or cancer. It may be used to diagnose cirrhosis or liver fibrosis when a previous injury or illness, such as long-term alcohol abuse or hepatitis, has completely scarred the liver. It may also be used, for example, in the case of hepatitis, to determine how well the patient responds to care.
- Infection: A needle biopsy will help decide whether an infection is present and what kind of organism is causing it.
- Inflammation: The doctor may be able to assess what is causing the inflammation by analyzing the cells in, for example, a needle biopsy.
Biopsies are often performed on transplanted organs to assess if the organ is being rejected by the body or if a disease has come back that made a transplant possible in the first place.
If a lump or tumor is present, it can be removed as part of a biopsy procedure at the same time.
Review and outcomes
Depending on the kind of biopsy, how long it takes to get the results will vary. Within 2 to 3 days, a simple outcome may be ready, but a more complicated case may take 7 to 10 days.

The tissue samples are sent to the laboratory where a pathologist tests them. They can be treated chemically and sliced into very thin sections. Under a microscope, they are normally examined. A blood specialist may also research the sample, or a hematologist.
The thin slice is attached to a glass slide and, for further studies, the remaining tissue is usually saved.
The slide has dyes applied to it often. These stain the tissue, and this allows the pathologist to more easily see the cells.
The pathologist would need to decide whether the sample is malignant, meaning cancerous, or benign in cases of cancer. They will decide how dangerous or advanced the cancer is because it is malignant. There are special stains that can be done to help direct care and prognosis if it is cancer.
Finally, a report that contains any abnormal or relevant findings is prepared by the pathologist. This report will be submitted to the physician who requested the biopsy.
The time it takes to get the results depends on the type of tests that are needed.
To collect the results, the patient would usually need to make another appointment with the doctor. This will extend the processing period for the findings if many experiments are carried out.
What to expect
A biopsy is an outpatient procedure in most cases, and the patient can go home immediately or very soon after it is finished.
Preparation is based on the biopsy type. There will not be any special training for a fine needle biopsy that is performed in the doctor’s office.
In order to claim they agree to the operation, the patient may need to sign a consent form and they will have to wear a gown instead of their own clothes.
The patient should not eat or drink beforehand in certain cases and should check with the doctor whether they should take their regular medications or supplements or not.
Sometimes, with or without a drug, a local anesthetic will be used to assist relaxation during the process.
The patient may require general anesthetic and may have to remain overnight in the hospital if a sample is to be taken from an internal organ. Otherwise, they can use a local anesthetic.
It normally takes no anesthesia to scrape a tissue sample from, for example, the inside of the mouth, but the area may feel sore for a while.
Often, it is essential to stitch an incision and a dressing may be necessary.
A patient who has a sample taken from a large organ, such as the liver or kidneys, may have to rest for a few hours in the hospital before going home.
There may be minor vaginal bleeding after a sample is taken from the womb lining or cervix.
Is it painful?
There should be no discomfort during the operation if anesthesia is used, but during the initial injection, there may be a skin prick.
A pin prick and a sharp pinch are felt during a needle biopsy.
For a few days, depending on the type of biopsy, there might be some soreness.
Is it safe?
Typically, a biopsy is healthy and it is known to be a very low risk procedure. There is a slight possibility of infection, as with any skin perforation, but the risk of an infection needing antibiotic treatment is possibly smaller than 1 in 1,000.
Occasionally, accidental injury may affect nearby organs, such as bowel damage during an abdominal biopsy.
Complications include the risk of bleeding, the absence of a suspicious tissue site that could lead to a false negative result, and the failure to obtain sufficient material so that the biopsy has to be replicated.
One research into the effects of biopsies used in clinical trials showed that complications contribute to 5.2 percent of those biopsies.
A breast biopsy research has shown that cancer cells will break away from a lump, spreading the disease to other regions.
Other studies into pancreatic cancer biopsies, meanwhile, concludes that the risk of mortality is not increased by endoscopic ultrasound-guided fine needle aspiration.
A biopsy may provide an early diagnosis of cancer and other diseases, whatever the risk, and early detection is crucial in many cases to increasing survival rates.
Sources
- Biopsies. (2015, June 19)
(LINK) - Biopsy. (2015, November)
(LINK) - Biopsy. (n.d.)
(LINK) - Breast biopsy. (n.d.)
(LINK) - Hansen, N.M., Ye, X., Grube, B/J., & Giuliano, A.E. (2004, June). Manipulation of the primary breast tumor and the incidence of sentinel node metastases from invasive breast cancer. Archives of Surgery 1396: 634-9
(LINK) - Biopsy: What you need to know (LINK)
- NCI dictionary of cancer terms. (n.d.)
(LINK) - Ngamruhengphong, S., Swanson, K.M., Wallace, M.B. (2015, July). Preoperative endoscopic ultrasound-guided fine needle aspiration does not impair survival of patients with resected pancreatic cancer [abstract]. Gut
(LINK) - Overmann, M.J., Modak, J., Kopetz, S., Yao, J.C., Hicks, M.E., Abburzzese, J.L., & Tam, A.L. (2013, January). Use of research biopsies in clinical trials: Are risks and benefits adequately discussed? Journal of Clinical Oncology 17-22
(LINK)