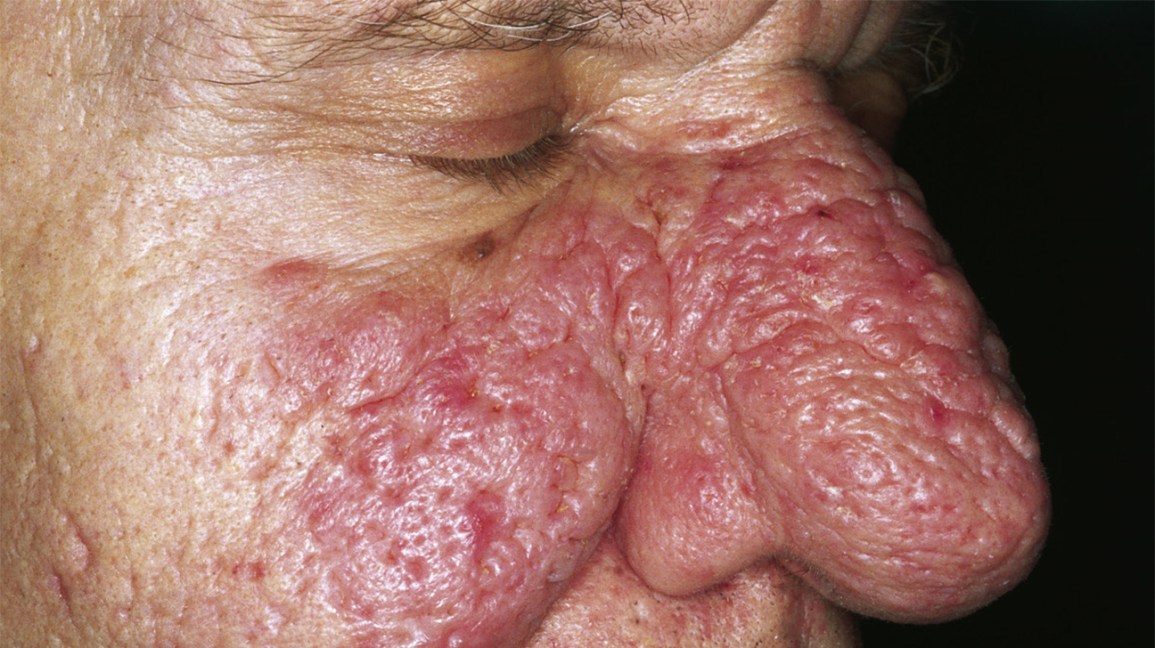
Rhinophyma is a skin condition that causes the nose to expand. Lumpy, thicker skin and fractured blood vessels are some of the other signs.
Males are far more likely than females to get the condition, which usually occurs between the ages of 50 and 70.
Researchers aren’t sure what causes it, but they do know that acne rosacea, which causes inflammatory pimple breakouts, is a precursor.
When acne rosacea advances to rhinophyma, the skin around the nose swells and the tip of the nose becomes larger. A diagnosis is made based on this distinctive appearance.
In the early stages, medicines are used, but in the latter stages, surgery is required. This is due to the possibility of damaged tissue obstructing the airways. The technique is safe and effective at smoothing or removing rough, thickened patches of skin.
Continue reading to find out more about the causes, symptoms, diagnosis, and treatment of this condition.
Causes of rhinophyma
Rhinophyma is characterized by an increase in the number of sebaceous glands (oil glands) and underlying connective tissues in the face. According to studies from 2021, the actual cause is still unknown, and various causes could be involved. A variety of disorders affecting the immune system, nerves, and blood arteries are included.
Acne rosacea, a long-term skin condition more common in women, is the prelude to rhinophyma. Rhinophyma develops in a subset of acne rosacea people.
Rhinophyma is more common in men, with a male-to-female ratio ranging from 5:1 to 30:1, and it usually develops in people between the ages of 50 and 70. Scientists believe that male hormones raise the danger because of the higher prevalence in men.
Some people believe that drinking alcohol causes the condition, however studies show that this is not the case. However, both alcohol and caffeine enlarge blood vessels briefly, aggravating rhinophyma.
In its early beginnings
According to evidence, rhinophyma begins as “pre-rosacea,” with face flushing being the only symptom.
The condition progresses to vascular rosacea, which is characterized by enlarged blood vessels and redness. Acne rosacea causes later, resulting in inflammatory outbreaks.
Finally, acne rosacea progresses to late-stage rosacea, which includes rhinophyma.
Symptoms
The first symptom of rosacea is frequently excessive face flushing. If it evolves to rhinophyma, a person may experience the following symptoms:
- thickened skin on the nose and elsewhere on the face
- expansion of the tip of the nose
- a bumpy texture on areas of the face
- enlarged pores
- oily skin
The condition may restrict the airways at this moment. In addition, because the fluid from the sebaceous glands thickens and can contain bacteria, persistent infection is common.
The amount of sebaceous glands and connective tissue alterations grow with time, resulting in increasing deformity.
Furthermore, there is a relation to cancer. Basal cell carcinoma affects 3–10% of people with rhinophyma, despite the fact that the condition is initially benign.
Diagnosis
Rhinophyma is often diagnosed with a visual examination due to its distinctive look.
The presence of at least one primary feature and at least one secondary feature is used by doctors to make a diagnosis.
The following are the main characteristics:
- blushing
- persistent redness
- pustules, small pimples containing pus
- papules — small, solid pimples that are usually inflamed but do not produce pus
- broken or dilated blood vessels near the skin’s surface
Secondary features include:
- roughened patches of skin on the face
- swelling
- burning or stinging areas of the skin
- eye symptoms, such as watery eyes or swelling of the eyelids
- marked thickening of skin or excess tissue
- these symptoms elsewhere on the body
Treatment
There are nonsurgical and surgical options available.
Non-surgical options
Certain drugs appear to be beneficial, according to the findings. Topical metronidazole (Metrocream) is one option for reducing skin inflammation by preventing the production of reactive oxygen species.
Isotretinoin, a medicine that shrinks the sebaceous glands and reduces the amount of oil they produce, is another choice. If a person wants surgery, however, they must stop taking this drug.
Surgical intervention
Advanced rhinophyma necessitates surgical removal of the afflicted tissue. A report published in 2020 describes a five-step surgical procedure for rhinophyma that is both safe and effective:
- Dermabrasion: A motorized device resurfaces the skin to facilitate the next steps.
- Dermaplaning: This involves removing affected tissue without directly cutting it. It prepares the skin’s surface for the third step.
- Debulking: The surgeon uses curved scissors to cut away the thickened skin. They also take samples of any areas that may be malignant and send them to a lab for analysis.
- Electrocautery: This involves using heat to destroy the affected tissue.
- Laser use: This final step seals and micro-contours the wound.
Although little data suggests that rhinophyma can recur following surgery, few long-term studies have been conducted.
Conclusion
A person with rhinophyma may suffer significant face flushing in the early stages. Swollen blood vessels and acne-like blemishes occur as the condition worsens.
Later on, the nasal skin thickens and the tip of the nose expands. Doctors diagnose rhinophyma at this point. It appears to be harmless at first, but it has the potential to obstruct airways and raise the risk of skin cancer.
Surgical and drug-based treatments can help, although there is limited evidence that the condition will reoccur after surgery.
Sources
- https://www.aao.org/eye-health/diseases/ocular-rosacea-facts
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7339328/
- https://www.ncbi.nlm.nih.gov/books/NBK544373/
- https://www.medicalnewstoday.com/articles/322166
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4426765/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5828925/
- https://www.aad.org/public/diseases/rosacea/what-is/symptoms