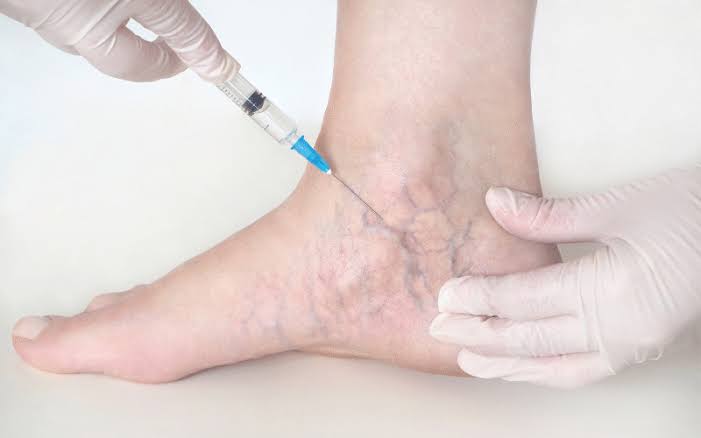
Sclerotherapy is a method of therapy in which a doctor injects drug into blood vessels or lymph vessels that tends to cause them to shrink. It is frequently used to help treat varicose veins or so-called spider veins.
The treatment is non-surgical, involving an injection only. It may also be used to treat diseases of the blood and lymph vessels that cause these vessels to improperly shape.
An irritating solution called a sclerosant, which is inserted directly into a vein or lymph vessel, is used in sclerotherapy. The vessel is irritated by the solution, causing it to swell. The blood or lymphatic fluid supply is cut off by this swelling and the vessel shrinks.
Since the 19th century, different types of sclerotherapy have been around, but techniques have advanced in recent decades.
We look at the uses of sclerotherapy in this article, what to expect from this treatment, and also during the recovery time.
What disorders are treated with sclerotherapy?

To treat varicose veins, sclerotherapy is most commonly used. Chronic venous insufficiency is also known as varicose veins.
Varicose veins arise when the veins swell and bulge, commonly in the legs. This is due to weak walls of the veins that, in turn, weaken the valves of the veins. As a consequence, the veins are filled with blood, causing them to swell and appear different.
Varicose veins may also be painful and can cause skin problems, including rashes. Sclerotherapy decreases the symptoms of vein damage by narrowing the veins, which makes varicose veins less visible and less painful.
Some other conditions are also treated with sclerotherapy, including:
- Malformed lymph vessels. These are vessels that carry lymphatic fluid or lymph, which helps the immune system fight infections.
- Hemorrhoids. When other therapies fail, sclerotherapy can be used. Hemorrhoids happen when the blood vessels around the rectum swell and become irritated, causing discomfort and painful bowel movements.
- Hydroceles. In a body cavity, a hydrocele is an unhealthy growth of fluid. Hydroceles are common in the testicles.
When to think of sclerotherapy
The treatment is not required for anyone who has spider veins or any disorder that can be treated with sclerotherapy. To decide if it is appropriate, people should discuss their symptoms and treatment options with their doctor.
There could be more affordable and less invasive options for other treatments. For instance, hemorrhoids also respond well to non-prescription treatments. This can include improvements in lifestyle, such as consuming more fiber and not straining when a bowel movement happens.
Sclerotherapy should be considered by people with spider veins when:
- the veins are painful
- The legs feel sore or heavy,
- The skin is patchy or dry on the legs or feet,
- A rash develops along the veins,
Things to expect
In order to examine the troublesome vein or lymph vessel, sclerotherapy requires consultation with a doctor. Spider vein sclerotherapy is normally done in a dermatologist’s or a vein specialist’s clinic.
Anesthesia or other special preparation is typically not needed for the procedure. Before surgery, people should obey the doctor’s orders, as lotions or oils may need to be avoided beforehand.
The person lies on their back with their legs up during the procedure. The region gets cleaned by a doctor, then a small needle gets inserted into the vein. The needle may pinch.
The doctor injects the vein with an irritating solution. The person can feel burning, tingling, or nothing at all at all.
When the injection is complete, to prevent blood from re-entering the vein, the doctor will rub the area. The person may need to wear a pad or compression stockings in the area.
In most cases, in order to collapse a vein entirely, someone would require follow-up treatment. If many varicose veins are present, the only way to get rid of them could be through multiple treatments.
Following care, people should stay vigilant to avoid the development of blood clots. Sunlight, which can create dark spots in the treated area, would still need to be avoided by most.
At the site of the injection, some people experience tenderness or bruising, but recovery is otherwise reasonably simple.
Risks
A secure treatment is sclerotherapy. As it does not require anesthesia, it is a less invasive and dangerous choice than surgery.
Research shows that in 75-90 percent of cases, it eliminates spider veins successfully, but usually requires several procedures. Additional therapies, like surgery, may be required when sclerotherapy does not work.
Bruising, redness, and discomfort near the injected vein are among the most common negative reactions to sclerotherapy. About a third of people develop small branches of blood vessels surrounding the injected vein. Usually, these vessels disappear on their own.
A person can experience allergic reactions to the solution, burning of the vein, and changes in skin color less frequently.
Tiny air bubbles can also reach the bloodstream from the needle, causing changes in vision, headache, and nausea.
Very rarely, in the treated vein, a blood clot can form. If left untreated, blood clots may move to areas of the body and become life threatening. It can cause an embolism if a blood clot moves.
If they experience chest pain, trouble breathing, or dizziness after sclerotherapy, people should seek emergency care.
Costs and coverage from insurance
Sclerotherapy insurance coverage depends on whether the treatment is judged by an insurer to be medically appropriate.
If spider veins are just a cosmetic issue, the treatment may not be protected by insurance. Some insurers may require individuals to try other treatments, such as cryotherapy to freeze the veins, before attempting sclerotherapy.
It is protected if it is medically required when sclerotherapy is used for another condition, such as hemorrhoids. This could require a physician to explain that other therapies have failed or that it is likely that sclerotherapy is the most safe and efficient treatment.
Alternatives

Not all veins that are malformed need treatment. When there are no other signs, it is safe to monitor the veins to see if they get worse or begin causing other symptoms.
Changes in lifestyle can prevent the veins from getting worse and prevent new varicose veins from forming. Other methods for treatment can include:
- cryotherapy or freezing the veins
- laser therapy, using light to fade the veins
- vein ablation, using heat on a malformed vein
- closing the vein with surgery
- surgically removing the veins in severe cases
Conclusion
Typically, sclerotherapy is a minor, noninvasive treatment for repairing troubled veins. The outlook for individuals after sclerotherapy is nice since serious side effects are rare and it is successful.
People who think about the dangers and benefits of sclerotherapy should speak to a doctor about the treatment and consider getting a second opinion. Contacting an insurer to learn if the treatment is covered is also prudent.
Sources
- Francis, J. J., & Levine, L. A. (2013, May). Aspiration and sclerotherapy: A nonsurgical treatment option for hydroceles [Abstract]. The Journal of Urology, 189(5), 1725–1729
(LINK) - Hager, E. S. (n.d.). Varicose veins
(LINK) - Henke, P. K. (n.d.). Chronic venous insufficiency
(LINK) - Lymphatic malformation treatment and recovery. (n.d.)
(LINK) - Mounsey, A. L., Halladay, J., & Sadiq, T. S. (2011, July 15). Hemorrhoids. American Family Physician, 84(2), 204–210
(LINK) - Sclerotherapy. (n.d.)
(LINK) - Sclerotherapy: Chemical injection treatment. (n.d.)
(LINK) - What is sclerotherapy?. (LINK)
- Veräjänkorva, E., Rautio, R., Giordano, S., Koskivuo, I., & Savolainen, O. (2016, November 23). The efficiency of sclerotherapy in the treatment of vascular malformations: A retrospective study of 63 patients. Plastic Surgery International
(LINK) - What causes varicose veins? (2014, February 13)
(LINK) - Worthington-Kirsch, R. L. (2005, September). Injection sclerotherapy. Seminars in Interventional Radiology, 22(3), 209–217
(LINK)