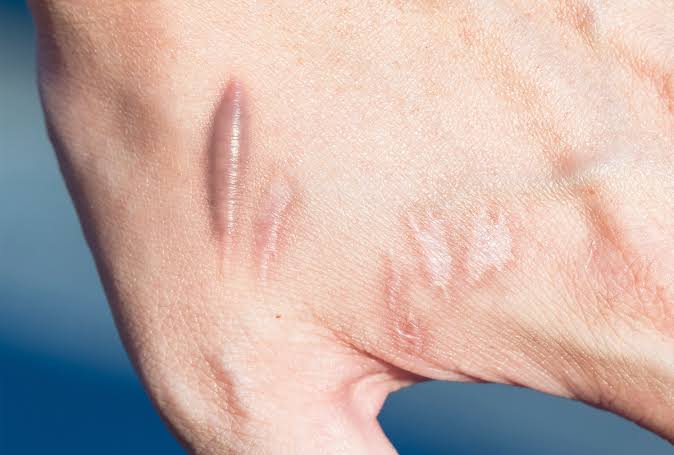
A mastectomy is a surgical procedure that typically results in scarring and is used to treat breast cancer. There are certain kinds of mastectomy that leave more scarring than others.
A surgeon extracts tissue from either or both breasts during a mastectomy, taking out only a section or the breast as a whole. Afterwards, the scarring depends on the place and form of incision that the surgeon makes.
Depending on the amount of breast tissue that needs removal, and whether a person requires reconstruction surgery afterwards, a surgeon may decide on the approach.
It can take months or even years for mastectomy scars to fade, but they never disappear completely. Reconstruction of breasts may enhance their appearance.
We look at various approaches to mastectomy in this article and how these impact scarring. We also clarify how post-mastectomy scars should be treated.
Different paths to incision

The appearance of a mastectomy scar will depend on the type of incision and surgical approach.
To start the operation, a surgeon may make an incision in the chest.
The surgeon removes breast tissue, muscles, and lymph nodes. The incision is then closed using stitches.
A scar can form over time. Some mastectomy scars heal in a horizontal line across the chest, a diagonal line, or often in a half moon shape.
The incision type and scar color depend on the position of the breast cancer lesion.
Medical treatments have greatly improved and a number of options are now available. People may ask their surgeon about procedure and its potential outcomes.
Which mastectomy will cause scarring?
The type of mastectomy performed on a patient can determine the degree of scarring.
Partial mastectomy or lumpectomy
It includes extracting the tumor and any underlying breast tissue. Often, the surgeon will also strip the covering of the chest muscles.
A lumpectomy will normally leave a small linear scar on the breast. A surgeon can conceal the scar in the crease of the breast or around the nipple.
A partial mastectomy leaves the majority of the breast intact, and reconstruction is not typically required.
As the size of the breast and amount of tissue removed varies, the size of the breast on the other side can differ.
The resulting breast might also have a divot or depression if it is small and the mass removed is particularly large.
Women who have a lumpectomy typically need radiation therapy.
Skin sparing mastectomy
For women who choose to continue the procedure with immediate breast reconstruction, a surgeon will normally prefer this technique.
Removing the breast, areola, nipple, and one or more lymph nodes requires a skin-sparing mastectomy. The surgeon can, however, preserve the remaining breast tissue.
Saving much of the breast skin enables the surgeon to begin immediate reconstruction from elsewhere in the body with an implant or tissue.
A skin-sparing mastectomy normally leaves the front of the breast with a visible, medium-to-large scar.
Nipple sparing mastectomy
A candidate for a nipple-saving mastectomy may be a person who is due to receive a preventive mastectomy or has early stage breast cancer. Preserving the skin and areola is part of this process.
This strategy would definitely favor women with smaller breasts. A scar on the side or at the base of the breast will result. Placing the incision under the breast in the crease may cover the scar further.
Simple or total mastectomy
A surgical approach that includes extracting the breast, areola, and nipple is this form of mastectomy. Often, if they show cancer symptoms, a surgeon will also remove the lymph nodes as well.
Depending on plans for reconstruction, they can also change the amount of breast skin they extract during the operation.
Usually, an oval shaped incision is made by the surgeon that goes around the nipple and around the width of the breast, leaving a prominent scar around the chest.
Modified radical mastectomy
This approach includes removing all breast tissue plus lymph nodes in the breast and armpit, similar to a simple mastectomy. Mostly, the surgeon leaves the chest wall intact.
A modified radical mastectomy will result in the chest getting a big, noticeable scar.
Follow-up treatments
The aim of a mastectomy or any oncological procedure is to remove just as much tissue as cancer requires to be treated, which will help to minimize any scarring.
The options will be explored by a breast surgeon to oncologist and help a person make the right decision in their case.
A woman will possibly have drainage tubes after surgery and require several weeks to recover.
Some procedures do not usually require a stay in the hospital, such as a lumpectomy. However, larger mastectomies also involve a stay in the hospital.
The duration of the hospital stay and length of recovery time are also determined by the form of mastectomy and reconstruction.
A doctor can prescribe radiation therapy or chemotherapy after a mastectomy to shrink the tumor or kill any remaining cancer cells. These treatments will influence the healing of wounds as well.
For signs of infection, such as warmth, redness, or discharge, a woman should track the wound. A fever may indicate a systemic infection as well.
Breast reconstruction
After a mastectomy, breast reconstruction is an alternative. The appearance of the breast or breasts is recreated by a surgeon, either at the time of the mastectomy or after healing.
Breast reconstruction will still cause scarring, but instead of a flat scar on the chest, it can lead to a more complete look at the breast. The procedure can also decrease a mastectomy’s psychological effects.
By removing tissue from another part of the body, using breast implants or both, a surgeon can accomplish the reconstruction.
Pictures
What if a woman does not choose reconstruction?
According to BreastCancer.org, an estimated 44 percent of women undergoing mastectomy do not opt to pursue the treatment with breast reconstruction.
Many women choose this course for different medical and personal reasons. Any of these may include:
- Health concerns that could make later surgeries dangerous
- The need to more rapidly resume daily operations
- Concerns about taking tissue or using an implant from other places
- Cost issues for individuals without insurance
Those that do not want to reconstruct may choose to wear a prosthetic or artificial breast that can be inserted into a bra. An elastic, breast-shaped system that fastens to the body is one alternative.
Women who do not choose one of these choices often refer to their choice as “going flat.”
Reducing scarring without reconstruction
They can consult with their doctor about surgical options if a person chooses against reconstruction, which may make the mastectomy scar and the resulting skin more comfortable.
A surgeon, for example, should ensure that the scar lies as flat against the chest as possible, which can help the chest feel smooth. Otherwise, a person with skin on their chest that bulges could be left by the surgery.
While this bulging is not physically detrimental, many individuals do not like its appearance.
A surgeon may often make what they call an incision of a “Y” or an anchor pattern. Two small incisions are applied to the end of the conventional long incision by this method, which may minimize bulging skin during the procedure.
Mastectomy tattoos
A report by a tattoo artist who collaborated with women to cover their mastectomy wounds with tattoos was published in the Journal of the American Medical Association in 2017.
This is an emerging technique for individuals who chose not to have breast reconstruction, which can be a choice.
Many people even want to have a tattoo artist draw a three-dimensional-looking nipple. Certain tattoo artists specialize in this approach.
Conclusion
An individual option is the choice of reconstructing a breast, covering a mastectomy scar, or living life without wearing a prosthesis. It is necessary for individuals to explore all these options with a surgeon.
If a person thinks that their desires for reconstruction are not valued by a doctor, they should want to get a second opinion.
An individual may also choose to delay any decision until after a mastectomy regarding the reconstruction process.
Sources
- Allen, D. (2017). Moving the needle on recovery from breast cancer. The healing role of postmastectomy tattoos [Abstract].
(LINK) - Bland, K., M., et al. (2017). The breast: Comprehensive management of benign and malignant diseases, 5th edition. Philadelphia, PA: Elsevier.
(LINK) - Breast reconstruction after mastectomy. (2017).
(LINK) - Breast reconstruction: Options after a skin-sparing mastectomy. (n.d.).
(LINK) - Going flat: Choosing no reconstruction. (2019).
(LINK) - Mastectomy. (n.d.).
(LINK) - Mastectomy. (2017).
(LINK) - What to expect after breast reconstruction surgery. (2017).
(LINK) - Medicalnewstoday – What to know about mastectomy scars (LINK)