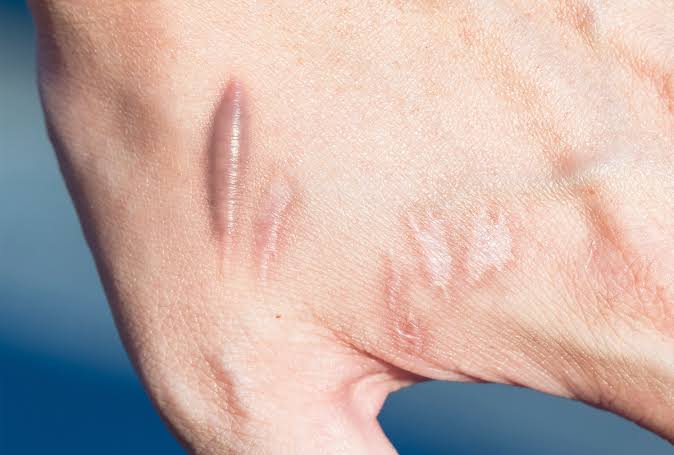
The body reacts when an individual has an injury by healing the damaged tissue, which creates scar tissue.
Scar tissue is a cell and collagen array that protects the injury site. As a result of an accident, surgery, or acne, people may grow scar tissue on their skin. Other parts of the body, such as the heart muscles following a heart attack, can also develop scar tissue.
In a variety of ways, scar tissue may occur, including:
A keloid is an elevated, red-skin colored plaque of scar tissue that after an injury can develop on tissues. Sometimes on the upper chest, shoulders, and upper back, keloids appear.
A more common type of scar tissue is a hypertrophic scar. People with hypertrophic scars will find that, over time, they fade.
A contracture scar typically occurs in tissues that have had a burn injury. The function of the affected region may be hampered by these scars.

While doctors remain unsure of what causes scar tissue to develop, they do know that burns, insect bites, acne, chicken pox, piercings, tattoos, and surgery can result in hypertrophic scars and keloids.
Researchers have also found that keloids in people with darker skin grow more frequently.
In younger individuals aged 10 to 30 years, both keloids and hypertrophic scars appear to occur more frequently.
Prevention is the most important guideline for scarring. If possible, people who have risk factors for developing irregular scars should avoid elective surgery and treat conditions such as acne that may result in scarring.
Sometimes, surgery is necessary.
At the position of the scar, people can feel itchiness and discomfort. Other scars are able to limit movements. Emotional and psychological discomfort from the presence of scars may be experienced by certain individuals.
To minimize the appearance of scarring, physicians should prescribe medications, but they must also address the psychological effect and physical constraints a scar can create.
Therapy
Researchers report that every year, scar therapies cost over $20 billion in the United States.
There are a number of therapies available for scars, but not all of them can be effective for all. It is necessary for doctors to clarify the limited efficacy of these procedures and to set realistic standards for the handling of scars by individuals.
Treatment options include:
- topical
- injectable
- cryotherapy
- radiotherapy
- laser therapy
- mechanical
Onion extract
Often, to prevent a scar from developing after surgery or laser tattoo removal, a doctor may recommend applying onion extract topically.
There may be anti-inflammatory properties of onion extract and the ability to destroy bacteria.
People typically tolerate onion extract well, but no clear evidence has been found by researchers that this treatment is successful. One research showed it was no better than an ointment dependent on petroleum, such as Vaseline.
Mitomycin C
Mitomycin C is a type of chemotherapy agent that has limited keloid treatment efficacy. The effectiveness of topical mitomycin C when used with other therapies, such as radiation therapy and surgical keloid removal, has been investigated in most studies.
For scar control, researchers do not recommend mitomycin C because there is not enough credible evidence to support its use.
Imiquimod
Imiquimod is available in a 5 percent cream formulation. Some physicians recommend imiquimod cream following surgical removal to individuals with keloids. Once again, in clinical trials for the treatment and prevention of keloid scar development, this topical treatment has not produced consistent results.
Bleomycin
To stop the development of collagen at the site of the injury, some doctors might inject bleomycin into the scar. The influence of injectable bleomycin on improving the appearance of hypertrophic scars and keloids has been evaluated in only a few studies.
Some researchers have found that the redness, itchiness, and pain associated with these scars may also be reduced by bleomycin.
Bleomycin is a treatment that is used in cancer treatments by doctors. It is a toxic substance, but by injecting it into a scar, doctors rarely record toxic side effects.
Interferon
Interferon also affects collagen development, and it can be injected into damaged tissue by doctors. In clinical trials, researchers found that injecting interferon reduced the size of a keloid by 50 percent in 9 days. This creates an effect that is more important than injecting a corticosteroid.
A further research found that the consistency and volume of the scar increased after injecting interferon into a hypertrophic scar.
Usually, physicians do not use interferon because it is costly, and existing research is not sufficiently good to justify its use. It also needs three injections a week, which for certain individuals can be inconvenient.
Corticosteroids

As the first alternative for treating keloids and the second choice of treatment for hypertrophic scars, physicians prefer corticosteroid injections. Doctors use triamcinolone acetonide, which is a corticosteroid that is injectable.
The prescribed dosing schedule may vary, but three to four injections every 3 to 4 weeks are involved in a typical injection schedule. More than four injections may be needed by some individuals. Researchers have shown that between 50 and 100 percent of individuals responded to the procedure.
To improve the thickness of a scar and minimize itchiness, some doctors can prescribe triamcinolone acetonide injections along with cryotherapy.
Botulinum toxin A
For several years, several clinicians have been injecting botulinum toxin A to prevent and treat scars, but studies have found contradictory proof of its efficacy in scar management.
Cryotherapy
Cryotherapy involves cooling body tissue to below zero temperatures using liquid nitrogen. This appears to be having an effect on the treatment of scars. By affecting the underlying scar tissue, this procedure can have the advantage of enhancing the appearance of scars.
Some studies have recorded a 51 percent reduction in scar volume after one operation, but other experts agree that cryotherapy is more successful when used in conjunction with other therapies, such as injectable corticosteroids.
Radiotherapy
Along with other scar treatments, physicians can use radiotherapy. Usually, after having a keloid removed, individuals will undergo radiotherapy to decrease the development of another keloid.
Radiation can help decrease cell growth and prevent the deposition of collagen in the damaged tissue.
Doctors advise about the use of radiotherapy for scars on the neck or chest because as a result of the radiation, there is an increased risk that a person may develop thyroid or breast cancer.
Laser therapy
To treat scar tissue, there are two types of laser therapies: ablative and nonablative. Ablative laser treatment is used by a doctor to flatten scar tissue. Non-ablative laser therapy will interrupt the scar tissue’s blood flow, which ultimately destroys the abnormal tissue.
Overall, researchers have shown that positive outcomes for surgical scars, hypertrophic scars and keloids are shown by laser therapy.
People can notice changes in the thickness of the scar, redness, itchiness, and texture when a doctor chooses the right form of laser therapy.
Silicone treatments
For scar control, physicians often prescribe silicone treatments. People can notice an improvement in the volume, elasticity, color, and firmness of hypertrophic scars and keloids after using silicon-based treatments.
Various silicone treatments are available, such as silicon gel sheet and creams that people can apply to the scar for 12 hours a day. Before seeing any effects, people can need to use the medication for 12 to 24 weeks.
Pressure therapy
Individuals may apply dressings that apply pressure on the scar tissue. Mechanical pressure will also decrease the scar tissue’s blood flow, which can help to flatten the scar.
These dressings are painful, and individuals need to wear them for 6 months for at least 23 hours a day.
Unfortunately, researchers have shown that only minor changes in scar height can be provided by pressure therapy.
Adhesive microporous hypoallergenic paper tape
Researchers also found that individuals in a region of the body that is under elevated skin tension have a higher risk of developing a hypertrophic scar. A non-stretch adhesive microporous hypoallergenic tape is another strategy to reduce the development of scar tissue.
This tape can help to relieve tension around a wound and can avoid the development of scar tissue.
Is massage therapy helping?

Scar massage is a technique used in hospital burn units by healthcare professionals to enhance the function and appearance of scarring caused by burns. The proof is poor, but some experts claim that scar massage helps strengthen hypertrophic scars and maybe even avoid them.
Anyone considering massaging their scar, particularly if they have had stitches or other surgery, should first discuss it with a doctor.
The evidence supporting scar massage was tested by one study. While researchers need to conduct more research to validate these findings, researchers state that the following may be improved by scar massage on hypertrophic burn scar tissue:
- scar height
- pain
- depression
- itchiness
For researchers, there are no specific scar evaluation methods, and massage techniques can vary from one study to the next. Researchers need to perform controlled, clinical research on the efficacy of massage for scar tissue management.
Conclusion
In order to avoid and manage scar tissue, there are many different therapies that physicians can use. No treatment, however, is uniformly effective.
When treating scar tissue, doctors have several choices to choose from, but certain treatments for some forms of scars are more successful. The psychological effects and movement constraints that scars can affect certain individuals should also be discussed by doctors.
Doctors should inform people of the often limited success rates of scar tissue therapy and set realistic goals with them.
Sources
- Ault P, et al. (2018). Scar massage for hypertrophic burns scarring – a systematic review [abstract].
(LINK) - Block, L., et al. (2015). Emerging therapies for scar prevention.
(LINK) - Carswell, L., & Borger, J. Hypertrophic scarring keloids. (2019).
(LINK) - Keloids and hypertrophic scars. (n.d.).
(LINK) - Mostaco-Guidolin, L., et al. Imaging collagen in scar tissue: Developments in second harmonic generation microscopy for biomedical applications. (2017).
(LINK) - Oosterwijk, A. M., et al. (2017). Prevalence of scar contracture after burn: A systematic review [Abstract].
(LINK) - Owji, N., et al. (2018). Effectiveness of topical onion extract gel in the cosmetic appearance of blepharoplasty scar [Abstract].
(LINK) - Prohaska, J., & Badri, T. Cryotherapy. (2019).
(LINK) - Shin, T. M., & Bordeaux, J. S. (2012).The role of massage in scar management: A literature review [Abstract].
(LINK) - Ward, R. E., et al. (2019). Surgical and noninvasive modalities for scar revision [Abstract].
(LINK) - Medicalnewstoday – What to know about scar tissue (LINK)